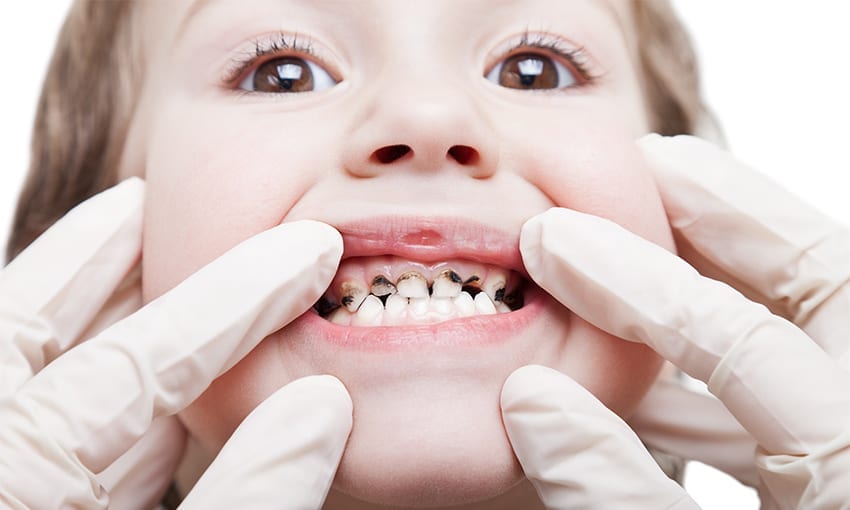
ECC Dental Treatment in East Gosford, Central Coast, NSW.
This blog provides detailed information about early childhood caries, which we hope you find helpful.
Regular dental check-ups and cleans are important to help keep your child’s teeth healthy. At VC Dental, we are experienced in dentistry for young children and we provide a range of preventative services at our modern clinic in East Gosford on the Central Coast. If you are interested in our early childhood examinations, please click this link to visit our children’s dentistry services page instead.
Did you know that dental decay is the number one chronic infectious disease in children? This is a worldwide public health concern affecting both industrialised and developing nations. There are both immediate and long-term effects of the disease. It can also have a substantial impact on the children’s’ families both socially and economically1.
What is Early Childhood Caries (ECC)?
ECC goes by many other names. It has been referred to as baby bottle decay, baby bottle caries, nursing caries, and bottle rot amongst other names. ECC is defined as the presence of one or more decayed, missing (due to decay), or filled tooth surface/s in any primary (baby) tooth in a child up to the age of 6. However, ECC generally refers to a specific pattern of decay observed along the gum line in the baby teeth of children. The teeth most affected are usually the four upper incisors (the four front teeth)2.
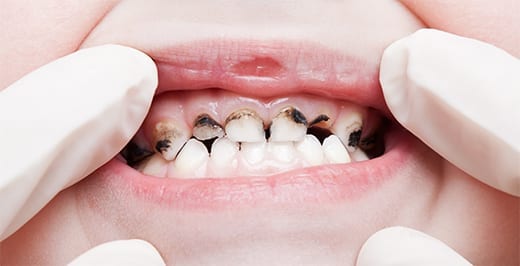
Specific gumline decay
What causes ECC?
There are several risk factors which play key roles in the progression of the disease, but it basically boils down to poor diet and poor oral hygiene3.
1. The bacterial risk factor

There are two main bacteria identified in the progression of the disease: Streptococcus mutans and Streptococcus sobrinus. These two bugs LOVE sugar. They consume whatever sugar is left behind on your teeth and produce lots of tooth dissolving acid as a waste product.
According to the studies, S.mutans can make up 30% of the bacteria in the plaque scraped off teeth in children with ECC whereas it only makes up less than 0.1% in children with negligible or no decay4.
2. The sugar risk factor:
It surely comes as no surprise that sugary food and drink increases your chances of tooth decay, especially if the sugar is not being removed properly5.
3. The feeding risk factor

Inappropriate use of the baby bottle contributes significantly to the cause and severity of ECC. Examples of this are filling bottles with fruit juice, cordials or soft drink, and dipping bottle or dummy teats in syrups like honey.
When a child sips from a cup, the sugar moves past the teeth quickly and does less harm, but when a bottle is sucked slowly the sugar lingers in the mouth.
Prolonged bedtime bottle use and sleeping with the bottle, especially with sweet drinks, has been associated with severe ECC. Although milk and formula are technically not sweet drinks, they contain the sugar lactose. The bacteria in your mouth can breakdown this sugar and release plaque acids in the process6.
How is ECC treated?
Treatment depends on the severity of the disease. If we can catch ECC in its early stages, all that may be required is routine check-ups and cleans and better oral hygiene practices at home. If it’s a bit more severe, fillings or stainless-steel caps may be required. Sometimes partial or complete removal of the pulp may be necessary prior to restoration. And unfortunately, if the tooth is too far gone, then removal of the remaining tooth may be our only option7.
How can we prevent ECC?
There is no substitute for a healthy diet and good oral hygiene practices including routine dental visits.
We also want to avoid decay promoting behaviors8:
- Children should not be put to bed with a baby bottle containing anything but cool, boiled water. Even natural sugars found in milk and formula are harmful when they cling to a child’s teeth for a long period of time. The flow of saliva also decreases during sleep which usually helps to wash away sugars.
- “At will” breastfeeding should be avoided after the first baby tooth erupts and other dietary carbohydrates are introduced.
- Infants should be weaned off the bottle at 12 to 14 months of age; however you can begin to introduce a feeding cup from 6 months.
- Infants should be encouraged to use a cup as they approach 12 months of age.
- Constant sipping of sugary drinks or constant snacking on sugary foods throughout the day should be avoided.
Also interesting to note is that genetic research has identified that Streptococcus mutans is generally passed on from the caregiver to the infant around the time their first baby teeth erupt. In most cases the infant will have the same strain as the mother as they are usually the primary carer9. Therefore, it is beneficial for expecting mothers or women planning to conceive to make sure their mouths are healthy and free of any plaque, tartar, or decay10,11.
For more information you can read about Children’s Preventative Care here.
References:
1. Inglehart MR, Filstrup SL, Wandera A. Oral health and quality of life in children. In: Inglehart M, Bagramian R, editors. Oral health-related quality of life. Chicago: Quintessence Publishing Co; 2002. pp. 79–88
2. Drury TF, Horowitz AM, Ismail AI, Maertens MP, Rozier RG, Selwitz RH. Diagnosing and reporting early childhood caries for research purposes.A report of a workshop sponsored by the National Institute of Dental and Craniofacial Research, the Health Resources and Services Administration, and the Health Care Financing Administration. J Public Health Dent. 1999;59:192–7.
3. Berkowitz RJ. Causes, treatment and prevention of early childhood caries: A microbiologic perspective. J Can Dent Assoc. 2003;69:304–7.
4. Loesche WJ. Nutrition and dental decay in infants. Am J Clin Nutr. 1985;41:423–35.
5. Harel-Raviv M, Laskaris M, Chu KS. Dental caries and sugar consumption into the 21st century. Am J Dent. 1996;9:184–90.
6. Hallett KB, O’Rourke PK. Early childhood caries and infant feeding practice. Community Dent Health.2002;19:237–42.
7. Tinanoff N, Douglass JM. Clinical decision-making for caries management in primary teeth. J Dent Educ. 2001;65:1133–42.
8. Policy on early childhood caries (ECC): Classifications, consequences, and preventive strategies. Pediatr Dent. 2008;30:40–3.
9. Ercan E, Dulgergil CT, Yildirim I, Dalli M. Prevention of maternal bacterial transmission on children’s dental-caries-development: 4-year results of a pilot study in a rural-child population. Arch Oral Biol.2007;52:748–52.
10. Kishi M, Abe A, Kishi K, Ohara-Nemoto Y, Kimura S, Yonemitsu M. Relationship of quantitative salivary levels of Streptococcus mutans and S. sobrinus in mothers to caries status and colonization of mutans streptococci in plaque in their 2.5-year-old children. Community Dent Oral Epidemiol.
11. Kishi M, Abe A, Kishi K, Ohara-Nemoto Y, Kimura S, Yonemitsu M. Relationship of quantitative salivary levels of Streptococcus mutans and S. sobrinus in mothers to caries status and colonization of mutans streptococci in plaque in their 2.5-year-old children. Community Dent Oral Epidemiol.